1. Main points
The annual average growth rate of public service healthcare productivity from 1996 to 2013 was 0.8% per year compared with the previously published annual average growth for 1996 to 2012 of 0.7%
In 2013, productivity grew by 2.9% due to output growth of 4.5% outstripping input growth of 1.6%
This is the fourth consecutive year of positive productivity growth and the second-highest annual growth rate in productivity across the series, with the highest being 3.0% in 2011
The quality adjustment added 0.2 percentage points to output growth in 2013, compared with the average annual quality adjustment of 0.4 percentage points since 2001 when the quality adjustment was first applied
Strong output growth in 2013 was driven by an increase in activities for hospital and community health services
The continuing recent trend of low inputs growth was driven by low growth in labour and goods and services components
Figure 1: Public service healthcare output, inputs and productivity indices and growth rates, 1995 to 2013
United Kingdom
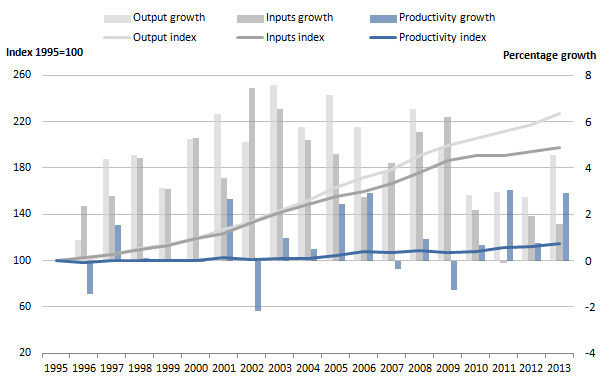
Source: Office for National Statistics
Download this image Figure 1: Public service healthcare output, inputs and productivity indices and growth rates, 1995 to 2013
.png (18.9 kB) .xls (29.2 kB)2. Introduction
This release contains updated estimates of output, inputs and productivity for public service healthcare in the UK between 1995 and 2012, and new estimates for 2013. Estimates are published on a calendar year basis to be consistent with the UK National Accounts.
Public service healthcare productivity is estimated by comparing growth in the total amount of healthcare output with growth in the total amount of inputs used. Productivity will increase when more output is being produced for each unit of input compared with the previous year. Estimates of output, inputs and productivity are given as both growth rates which show the change from the previous year, and as indices which show the overall trend over time compared with the base year in 1995.
Healthcare output is the quantity of healthcare delivered adjusted for the quality of delivery. The quantity is measured as the number of individual healthcare activities performed and quality of delivery is measured using a combination of indicators including survival rates, waiting times, primary care outcomes and results from the National Patient Survey. Healthcare inputs are composed of labour (measured as full-time equivalent staff numbers), goods and services, and consumption of fixed capital. Further information on methods, including information about data used for the different component countries of the UK and how these are aggregated to a UK index, is available in our sources and methods paper1.
Our public service productivity estimates were developed in response to the recommendations of the Atkinson Review2 on the measurement of government output and productivity for the National Accounts. Users of healthcare productivity estimates include the Department of Health and research organisations such as the Nuffield Trust and London School of Economics. Users may also be interested in similar estimates of the productivity of the healthcare system in England produced by the Centre for Health Economics at the University of York3.
It is important to note that while these productivity estimates provide a measure of the amount of output which is produced for each unit of input, they do not measure value for money or the wider performance of public healthcare services. They do not indicate, for example, whether the inputs have been purchased at the lowest possible cost, or whether the desired outcomes are achieved through the output provided.
The estimates in this release are subject to an open revisions policy, meaning that each time a new article is published revisions can occur for the whole of the time period. On this occasion there have been no major changes to the production of the estimates and minor revisions to estimates of output, inputs and productivity compared with previously published statistics are due to small changes in source data.
Notes for introduction
ONS (2013a) - Sources and Methods Public Service Productivity Estimates: Healthcare
Atkinson, T (2005) - Atkinson Review: Final Report. Measurement of Government Output and Productivity for the National Accounts, Palgrave MacMillan: UK (1.1 Mb Pdf)
Centre for Health Economics (2014) - Productivity of the English NHS: 2012/13 update, Centre for Health Economics, CHE Research Paper 110
3. Output quantity
Healthcare output is measured as the quantity of healthcare delivered adjusted for changes in the quality of delivery. The quantity of output is estimated by weighting the growth rates for thousands of individual healthcare activities by their proportion of total expenditure. The quantity of healthcare is estimated separately for each of the following sectors which are weighted together to produce an overall output quantity series:
Hospital and Community Health Services (HCHS) – includes hospital inpatient, outpatient and day case episodes
Family Health Services (FHS) – includes General Practitioner (GP) and practice nurse consultations, publicly funded dental treatment and sight tests
GP prescribing – includes all drugs prescribed by General Practitioners
Non-NHS provision1 – includes services provided by the private sector but funded by the government
Figure 2a shows the quantity output growth by component before it is weighted by expenditure share. Figure 2b presents this information after weighting, showing how growth in each component contributes to the growth in overall output quantity.
Figure 2a: Public service healthcare output volume growth by component, 1996 to 2013
United Kingdom
Source: Office for National Statistics
Notes:
- HCHS = Hospital and Community Health Services.
- FHS = Family Health Services.
Download this chart Figure 2a: Public service healthcare output volume growth by component, 1996 to 2013
Image .csv .xls
Figure 2b: Public service healthcare contributions to output growth by component, 1996 to 2013
United Kingdom
Source: Office for National Statistics
Notes:
- HCHS = Hospital and Community Health Services.
- FHS = Family Health Services.
Download this chart Figure 2b: Public service healthcare contributions to output growth by component, 1996 to 2013
Image .csv .xlsThe longer-term trend in the growth of Hospital and Community Health Services (HCHS) was largely consistent from 1995 to 2013 with average growth of 3.3% per year2. There was some volatility with a noticeably higher growth rate in 2013 of 5.3%, as well as 5.6% in 2005 and 6.5% in 2008.
These high growth rates can be traced back to high growth in particular activities within the HCHS sector for these years. On the outpatient side, these were activities such as Trauma and Orthopaedics, Urology, Cardiology, Dermatology and Oncology. There were also increases in long-stay inpatient cases, which could be due in part to an increase in "bed-blocking". This is a term used to describe a situation where hospital patients – in particular the elderly – are occupying a hospital bed which they don’t need, usually because their discharge has been delayed. A paper3 by the Centre for Health Economics at the University of York found that a 1% increase in the elderly (aged 65 and over) population increases the number of bed-days lost due to delays by about 1.7% to 2%. The context of an ageing population in combination with an increasing number of delayed discharges is likely to lead to growth in the number of long-stay inpatient cases.
HCHS has the largest expenditure share, accounting for around 60% of healthcare expenditure. Its large share means that growth in the HCHS sector was the dominant contributor to overall healthcare output growth since 2005, and higher growth rates in 2005, 2008 and 2013 are exaggerated in the weighted contributions to growth. In 2013, HCHS volume growth contributed almost three-quarters of total output growth, driving higher overall output growth compared with the previous three years.
There was a steady downward trend in the growth rates of GP prescribed drug activities over the series from a maximum of 14.2% in 2000 to 3.2% in 2011 at which it has levelled out. Growth remained at a similar level of 3.3% in 2013. This is partly due to the number of items prescribed growing at a slower rate than before and also expenditure falling as a result of reduced prices for drugs4 through negotiating discounts and increased use of generic (non-branded equivalent) drugs.
The expenditure share of GP prescribed drug activities saw a corresponding decline from around 19% in financial year 2000 to 20015 to 11.6% in 2012 to 20136. The combination of falling expenditure share and slower growth rates reduced the contribution of GP prescribing to overall output quantity growth from 2.7% in 2000 to 0.4% in 2013.
Growth in the FHS component was somewhat volatile until 2007; however, since then it settled at around 1 to 2% growth per year, in line with the annual average growth across the whole series of 1.9%.
The expenditure share for FHS of 17.7% combined with low growth rates across the series means its impact on overall output growth is small.
Whilst growth in non-NHS provision was historically quite volatile with a high of 42.3% in 1997, it stabilised in recent years following a rapid decrease in growth rates from 21.8% in 2007 to 7.4% in 2010. The expenditure share for non-NHS activity more than doubled since 1995 from less than 4% to just over 10% in 2013. A report by the British Medical Journal7 entitled "Outsourcing the NHS" corroborates the increase in non-NHS provision, presenting Department of Health figures which show that the proportion of the NHS budget spent on private healthcare providers has increased in a similar way from 2.8% in financial year 2006 to 2007 to 6.1% in 2013 to 2014. Nevertheless, non-NHS provision still occupied the smallest share in total expenditure, and so the high and volatile growth rates were reduced when weighted together with the other components and the contributions to growth were not more than 2 percentage points across the entire series.
Total output quantity
Public service healthcare output grew in all years across the series. The highest output growth rates were in the mid-2000s, with a high of 7.1% in 2003. Output growth of 4.3% in 2013 is equal to the annual average growth rate over the whole series from 1996 to 2013. This represented a return to the longer-term trend following slower output growth of less than 3% in the previous three years from 2010 to 2012.
Growth in the volume of healthcare provided should be seen in the context of an increasing UK population. Our most recent mid-year population estimates8 how that the UK population has grown by 10.2% between 1995 and 2013 at 0.6% per year on average; this is slower than the 4.3% average growth of healthcare output. The comparison is not very straightforward though, due to the complexities of changing population structure and demand pressures on the NHS, and the method through which activities are cost-weighted together to calculate output growth.
Notes for Output quantity
Non-NHS provision is measured indirectly using expenditure, and uses the inputs=output convention, meaning implicit productivity for the non-NHS component is zero.
Average growth rates for cumulative growth across multiple years are geometric means calculated using the formula: [(index in current year/index in base year)^(1/(current year – base year))]-1
Centre for Health Economics (2014) - Testing the bed-blocking hypothesis: does higher supply of nursing and care homes reduce delayed hospital discharges?
Nuffield Trust (2014) - Cost of Prescription Items in the UK
Expenditure shares are calculated from raw data in financial years. These contribute to overall indices which are subsequently converted to calendar years.
To calculate a Laspeyres index, expenditure shares from the previous year are used. For more information, see Methodology Notes: Annual chain-linking, Robjohns (2006)
British Medical Journal BMJ - Outsourcing the NHS
Population estimates for UK, England and Wales, Scotland and Northern Ireland, Mid-2014
4. Output quality
In line with the recommendations of the Atkinson Review1 a quality adjustment is applied to the estimate of healthcare quantity. The adjustment reflects two measures of quality:
the extent to which the service succeeds in delivering its intended outcomes:
a. for HCHS services, this is measured using short-term survival rates, health gain following treatment in hospital and changes in waiting times
b. for primary care, this is measured as the percentage of certain groups of patients meeting target ranges for cholesterol levels and blood pressure
the extent to which the service is responsive to users’ needs – National Patient Survey results are used to measure patient experience of hospital inpatient services, mental health services, primary care, outpatient, and accident and emergency services
The impact of the quality adjustment was positive in all years, with the exception of a small negative impact in 2001, the first year it was applied. On average from 2001 to 2013 the quality adjustment added 0.4 percentage points per year onto the output growth rate. In 2013, the impact of the quality adjustment was lower than average, contributing an extra 0.2 percentage points to the output growth, which is consistent with the generally decreasing impact of the quality adjustment in recent years. Whilst the average annual effect from 2001 to 2006 was 0.6 percentage points, the average from 2007 to 2013 reduced to 0.3 percentage points.
Figure 3: Public service healthcare quantity and quality adjusted output index and growth rates, 1995 to 2013
United Kingdom
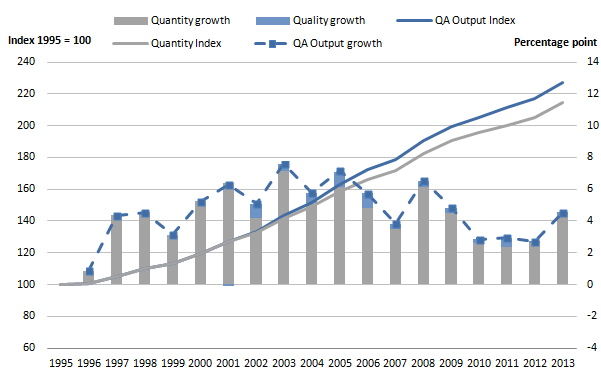
Source: Office for National Statistics
Notes:
- QA = Quality adjusted
Download this image Figure 3: Public service healthcare quantity and quality adjusted output index and growth rates, 1995 to 2013
.png (20.3 kB) .xls (28.7 kB)Notes for output quality
- Atkinson, T (2005) - Atkinson Review: Final Report. Measurement of Government Output and Productivity for the National Accounts, Palgrave MacMillan: UK (1.1 Mb Pdf)
5. Inputs
Inputs to publicly-funded healthcare are broken down into three components, weighted together using their share of total expenditure:
Labour - such as hospital consultants, registrars, nurses, technical staff, ambulance staff, support staff, General Medical Practitioners (GPs) and practice staff
Goods and services - such as non-staff costs of pharmaceutical services, dental and ophthalmic services, and the purchase of equipment by hospitals and GP practices which could include things like gloves and syringes; this component also includes GP prescribed drugs and services provided by non-NHS organisations
Consumption of fixed capital – the amount of capital stock, such as buildings and vehicles, used each year and is made up of depreciation and other capital charges
Estimates of labour inputs are based on direct measurement of the change in the number of full-time equivalent employees of the health service, weighted by their average salaries. Inputs for goods and services are estimated indirectly, using an appropriate deflator to remove the effects of price changes from current price expenditure. Capital consumption is measured using estimates from the UK National Accounts.
Figure 4a shows the inputs growth by component before it is weighted by expenditure share. Figure 4b presents this information after weighting, showing how growth in each component contributes to the growth in overall inputs.
Figure 4a: Public service healthcare input volume growth by component, 1996 to 2013
United Kingdom
Source: Office for National Statistics
Download this chart Figure 4a: Public service healthcare input volume growth by component, 1996 to 2013
Image .csv .xls
Figure 4b: Public service healthcare contributions to input growth by component, 1996 to 2013
United Kingdom
Source: Office for National Statistics
Download this chart Figure 4b: Public service healthcare contributions to input growth by component, 1996 to 2013
Image .csv .xlsBetween 1996 and 2010 the growth rate of labour inputs varied between 0.5% and around 5% with the highest growth rates in the period 2002-2004. Following renewed high growth rates of 4.3% in 2009 growth in labour inputs slowed considerably. The annual average growth rate for 2010 to 2013 was 0.1% compared with 2.1% across the whole series. Labour input growth in 2013 was more in line with the recent trend at 1.0%. The only fall in labour inputs was in 2011 of 1.0% caused by absolute falls in the number of healthcare staff, especially amongst administrative, support and senior managerial categories.
The share of expenditure for labour fell from 61.1% in 1995 to 51.5% in 2013. Reports by the Nuffield Trust1 have also shown how the proportion of expenditure on staff for Primary Care Trusts (PCT) has fallen in a similar way, from 56% of total expenditure in financial year 2003 to 2004 to 49% in 2012 to 2013. Growth in the volume of labour inputs was not high across the series, and so it was not the dominant contributor to growth despite it having the largest expenditure share. However, it did drive the fall in overall inputs in 2011.
Goods and services inputs had the highest annual average growth rate from 1996 to 2013 of 6.6%. However, growth slowed after 2009, with the annual average growth rate for 2010 to 2013 being 2.6%. Lower growth rates were caused by slower growth across several areas including administration and non-pay costs, as well as costs of the delivery of non-NHS services.
Goods and services accounted for the second-highest expenditure share (46.3%) in 20122, increasing from around 36% in 1995, reflecting the fall in the share of labour expenditure. Due to the growing share of total expenditure and the high volume growth rates, in every year except 2004 goods and services provided the largest contribution to the overall growth rate. In 2013, goods and services contributed 1.1 percentage points towards total inputs growth of 1.6%.
Capital consumption is the most volatile of the input components and it fell in every year from 2005. Capital inputs account for only 2% of expenditure, so whilst it experienced the largest recent decline in growth, its contribution to the level and volatility of total inputs growth was limited. The much greater shares of labour and goods and services mean that it is their contributions which largely drove the lower inputs growth in recent years.
Total inputs
Public service healthcare inputs grew in every year of the series, with the exception of 2011 which had a fall of 0.1%. The annual average growth rate of inputs from 1996 to 2013 was 3.8%. However, there was much lower growth in inputs after 2009 with an annual average growth rate over the period 2010 to 2013 of 1.4%. In 2013, inputs growth was 1.6%, which was the lowest in the series but for the fall in 2011.
The pattern of much slower inputs volume growth from 2010 onwards coincides with the Nicholson efficiency challenge3, which required the NHS in England to make £20 billion of savings by the end of the Spending Review period (2013). Alongside this, the NHS in England initiated the QIPP programme (Quality, Innovation, Productivity and Prevention) which had the aim of sharing good practice and providing tools for service providers to improve and streamline the provision of services to better meet patients’ needs. The recent much lower rate of real expenditure increases than have been seen in the past across the NHS are reflected in the statistics in this release showing historically small or zero volume increases in public service healthcare inputs for the years 2010 to 2013.
These initiatives also coincided with the Health and Social Care Act 20124, which introduced major reform to the local commissioning of services in England. Under this legislation, public health budgets transferred to local authority control, meaning services were commissioned locally rather than centrally. Public service healthcare inputs estimates are measured indirectly using overall expenditure on healthcare, and so this change in commissioning does not impact on the comparability of the year-on-year change in inputs.
Notes for inputs
Nuffield Trust (2014) - Into the red? The state of the NHS' finances - An analysis of NHS expenditure between 2010 and 2014 and Nuffield Trust (2013) - The anatomy of health spending 2011/12
To calculate a Laspeyres index, expenditure shares from the previous year are used and are therefore reported here. For more information, see Methodology Notes: Annual chain-linking, Robjohns (2006)
6. Productivity
Public service healthcare productivity is estimated by comparing change in the total amount of healthcare output with change in the total amount of inputs used. Productivity growth will occur when output growth is greater than inputs growth; that is, when more output is being produced for each unit of inputs compared with the previous year.
The size and direction of productivity growth has been variable over the series, though productivity increased in the majority of years, with an annual average growth rate in non-quality adjusted productivity of 0.5%, which increased to 0.8% when the quality adjustment was applied.
In the majority of years there was growth in both inputs and outputs, with years of productivity growth occurring when the volume of output grows faster than the volume of inputs. The largest fall in quality adjusted productivity in the series was in 2002 where large growth in inputs of 7.5% exceeded similarly high quality adjusted output growth of 5.1%.
Productivity has risen in all years from 2010 to 2013, though the size of the growth has been variable. Quality adjusted output growth remained just under 3% in all years from 2010 to 2012, with high productivity growth in 2011 caused by a small fall in inputs of 0.1%, compared with inputs growth of around 2% in 2010 and 2012. In 2013 higher productivity growth of 2.9% was a result of higher output growth of 4.5% while inputs growth remained relatively low at 1.6%. The impact of the quality adjustment on productivity was small in these years and did not change the direction of the trend, with the greatest increase being 0.6 percentage points in 2011.
Figure 5: Public service healthcare quantity and quality adjusted productivity index and growth rates, 1995 to 2013
United Kingdom
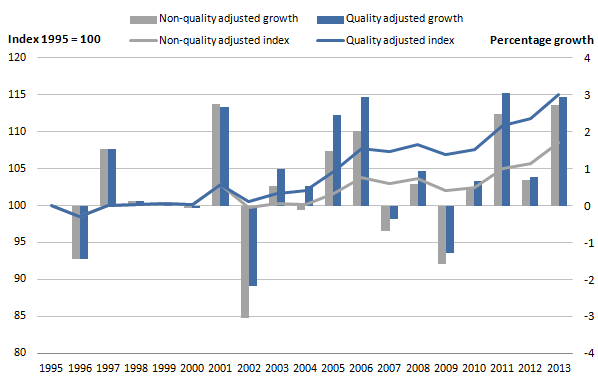
Source: Office for National Statistics
Notes:
- NQA = Non quality adjusted
- QA = Quality adjusted
Download this image Figure 5: Public service healthcare quantity and quality adjusted productivity index and growth rates, 1995 to 2013
.png (17.1 kB) .xls (28.2 kB)7. Revisions
In constructing the productivity index, revisions to data sources have led to minor revisions to previously published estimates of productivity growth. Figure 6 shows that revisions to productivity growth rates compared with those presented in Public Service Productivity Estimates: Healthcare 20121 are less then +/- 0.5 percentage points for every year in the series. There have been no changes to methods in this release compared with the previous publication.
Figure 6: Revisions to public service healthcare productivity growth rates, 1996 to 2012
United Kingdom
Source: Office for National Statistics
Download this chart Figure 6: Revisions to public service healthcare productivity growth rates, 1996 to 2012
Image .csv .xlsThe largest revisions are for 2008 and 2011 (-0.2 and -0.4 percentage points respectively). These are due to revisions in the output series, and can be attributed to updated figures2 for government expenditure by constituent country and also to changes in the estimates of unit costs for some elements of Family Health Services.
Notes for revisions
ONS (2015) - Public Service Productivity Estimates: Healthcare 2012
HM Treasury (2014) - Public Expenditure Statistical Analyses 2015

