Table of contents
- Main points
- Statistician’s comment
- Things you need to know about this release
- Life expectancy and healthy life expectancy in England, by the Index of Multiple Deprivation 2015 (IMD15), 2015 to 2017
- Life expectancy and healthy life expectancy in Wales by the Welsh Index of Multiple Deprivation 2014 (WIMD14), 2015 to 2017
- The Slope Index of Inequality for life expectancy and healthy life expectancy in England
- The Slope Index of Inequality for life expectancy and healthy life expectancy in Wales
- Comparing inequalities in life expectancy and healthy life expectancy between 2012 to 2014 and 2015 to 2017, England
- Comparing inequalities in life expectancy and healthy life expectancy between 2012 to 2014 and 2015 to 2017, Wales
- Quality and methodology
1. Main points
- In England, the gap in life expectancy (LE) at birth between the least and most deprived areas was 9.4 years for males and 7.4 years for females in 2015 to 2017; for healthy life expectancy (HLE) it was 19.1 years and 18.8 years respectively.
- In Wales, this gap in LE at birth was 9.0 years for males and 7.5 years for females in 2015 to 2017; for HLE it was 18.1 years and 19.4 years respectively.
- Since 2012 to 2014, there have been statistically significant increases in the inequality in LE in England for males and females at birth and at age 65 years; the inequality in female LE at birth had the largest growth, rising by 0.5 years.
- In England, the growth in the female inequality came from a statistically significant reduction in LE at birth of almost 100 days among females living in the most deprived areas between 2012 to 2014 and 2015 to 2017, together with an increase of 84 days in the least deprived areas.
- In Wales, the females living in the most deprived areas were expected to live up to 11 years more in a poorer state of health than their least deprived areas counterparts.
- In England, men resident in the least deprived areas could expect 13.3 years of good health from 65 years of age, but only 5.8 years if resident in the most deprived areas.
2. Statistician’s comment
“We’ve found a large fall in life expectancy at birth among women living in the most deprived areas in England when comparing the periods 2012 to 2014 and 2015 to 2017. This is in contrast to the continued increases in life expectancy for women living in the least deprived areas. This has led to a significant widening in the inequality in life expectancy at birth in England. Wales mirrored this pattern, although significant changes were not detected.”
“Our wider analysis of mortality shows that life expectancy in the UK has stopped improving at the rate that was expected before 2011. We will be carrying out further work to analyse the factors contributing to this trend, including the impact of deprivation.”
Ben Humberstone, Deputy Director for Health Analysis and Life Events, Office for National Statistics
Back to table of contents3. Things you need to know about this release
What has changed in this release?
In this release, we have:
- revised healthy life expectancy and disability-free life expectancy estimates using a new method of estimating health state prevalence estimates agreed following a consultation in December 2017 to February 2018
- revised estimates of life expectancy and health state life expectancy to take account of published revisions to Lower layer Super Output Area (LSOA) mid-year population estimates
- we have also changed the method for estimating the Slope Index of Inequality (SII) in life expectancy and health state life expectancy at age 65 years, by only including in the underlying population at risk those aged 65 years and over within the specific deciles; this has led to the SII estimates falling slightly compared with previously published estimates; the change also aligns the Office for National Statistics (ONS) with the method applied by Public Health England
- all estimates have been revised on the basis of these changes back to the period 2011 to 2013
What has changed since these statistics were designated as National Statistics?
Health state life expectancies were designated as a National Statistic in July 2012. Since then we have continually worked to develop the output to ensure it keeps up with user needs. In doing so we have implemented changes to enable Health State Life Expectancy to be estimated at sub-national level and be comparable across sub-national areas of the UK. We have had to adapt the data sources used due to decommissioning of the General Lifestyle Survey (GLF) in 2011. We have moved over to using the Annual Population Survey (APS) for the reporting period 2009 to 2011 onwards. Changing the source data gave us the opportunity to meet new user requirements:
- the requirement by the Department of Health and Social Care (DHSC) to include healthy life expectancy for upper tier local authorities in England as an over-arching indicator in the Public Health Outcomes Framework;
- the requirement by the DHSC to estimate the socioeconomic inequality in health state life expectancy in England as an over-arching indicator in the Public Health Outcomes Framework.
As the APS did not collect data for persons under the age of 16, we originally imputed the prevalence of younger ages based on the prevalence of those aged 16 to 19. This had been standard practice by ONS in historic series. In efforts to improve the limitations of this approach, we discussed with stakeholders the options for improving the approach to imputation. We agreed to use the proportional difference in health status found at Census 2011 to estimate the prevalence of those aged under the age of 16 and for those aged 85 years and over. Further details on the imputation method is available in the Health state life expectancies Quality and Methodology Information document. For the 2013 to 2015 release, through the UK Life Expectancy steering group, we agreed to extend the reporting of life expectancy and health state life expectancy from sub-national areas of England only to encompass sub-national areas of the UK. This was possible because health state prevalence estimation was available from the same data source and was therefore comparable.
A further refinement was tested out with stakeholders and consulted on in 2017 to model health state prevalence to improve the known relationship between health status and age, which for some sub-national areas did not always replicate this relationship because of sample size constraints. We produced an impact paper Proposed method changes to UK health state life expectancies using modelled health state prevalence and conducted a consultation on the proposed changes. The outcome was to implement the proposed changes, and further details of this method is available in the Health state life expectancies Quality and Methodology Information document.
What are health state life expectancies?
The life expectancy (LE) estimates reported in this release are period-based life expectancies. This is a measure of the average number of years a person would live from a given age, if he or she experienced the particular population’s age-specific mortality rates for that time period throughout his or her life. This measure makes no allowance for any future actual or projected changes in mortality.
Healthy life expectancy (HLE) is an estimate of the number of years lived in “Very good” or “Good” general health, based on how individuals perceive their general health. Disability-free life expectancy (DFLE) is an estimate of the number of years lived without a long-lasting physical or mental health condition that limits daily activities.
What are deprivation deciles?
National deciles of area deprivation are created through ranking small geographical populations known as Lower layer Super Output Areas (LSOAs) based on their deprivation score from most to least deprived and grouping them into 10 divisions based on the subsequent ranking.
Each decile represents approximately 10% of the population, with decile 1 being the most deprived LSOAs and decile 10 being the least deprived LSOAs. The exposure to deprivation lessens with each incremental move towards decile 10, so that residents of decile 2 areas are more deprived than those resident in decile 3, but less deprived than those resident in decile 1.
Deprivation deciles have been calculated separately for LSOAs in England and for LSOAs in Wales as their deprivation measures are derived differently and are not therefore comparable. For England, the Index of Multiple Deprivation 2015 (IMD15) was used as the measure of deprivation; in Wales, the Welsh Index of Multiple Deprivation 2014 (WIMD14) was used. The Quality and methodology section of this report details the domains each country’s IMD contains.
A back series of estimates using IMD15 and WIMD14 is provided in the datasets from 2011 to 2013, to 2015 to 2017 for life expectancy (LE) and healthy life expectancy (HLE) only. Even though there is no commentary in the bulletin, disability-free life expectancy (DFLE) data are included for the periods 2014 to 2016 and 2015 to 2017 only; the time periods are restricted due to changes from 2013 in the survey items used to produce statistical measures of disability.
How is inequality measured?
Inequality in this bulletin is measured in absolute terms using the range and the Slope Index of Inequality (SII). The range is the absolute difference between the most and least deprived deciles.
The SII can be interpreted in the same way as the range but takes into account inequality across the whole population as well as giving greater weight to larger populations and less weight to smaller populations. This means that the higher the SII, the more unequal the population is with regard to health outcome.
It is worth noting that Public Health England (PHE) also calculate the SII in life expectancy, which is published in the Public Health Outcomes Framework (PHOF) (PDF, 413KB) back to 2010 to 2012. Public Health Wales (PHW) also feature life expectancy and healthy life expectancy by measures of deprivation in their Public Health Outcomes Framework.
Back to table of contents4. Life expectancy and healthy life expectancy in England, by the Index of Multiple Deprivation 2015 (IMD15), 2015 to 2017
In England, the range in life expectancy at birth between the least and most deprived deciles was 9.3 years for males and 7.5 years for females in 2015 to 2017
Life expectancy (LE) at birth of males living in the most deprived areas in England was 74.0 years, compared with 83.3 years in the least deprived areas, nearly a decade difference (Figure 1). Males in the least deprived 50% of areas could expect to live beyond the age of 80 years, while those in the 50% most deprived fell short of 80 years.
Figure 1: Life Expectancy at birth 2015 to 2017: by sex and selected deciles, England
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 1: Life Expectancy at birth 2015 to 2017: by sex and selected deciles, England
Image .csv .xlsFemales in decile 1 could expect to live 78.7 years, while in decile 10 they were expected to live 86.2 years (Figure 1). Although females live longer than males in general, it was found that level of area deprivation exposure is important in modifying this general difference between the sexes in longevity. For example, these analyses have shown that males living in all four of the 40% least deprived areas (deciles 7 to 10) had statistically significant longer LE than females living in the 20% most deprived areas (deciles 1 and 2). The LE of the intervening deciles can be found in the datasets accompanying this release.
The largest gap between males and females occurred in decile 1 with a gap of 4.7 years, and smallest in decile 10 at 2.9 years. The sex-specific gap between adjacent deciles was largest between the two most deprived deciles, decile 1 and decile 2. Decile 2 males were expected to live more than 2.2 years longer than males in decile 1, showing a stark contrast even between relatively deprived populations. For females, the equivalent gap was 1.6 years.
In England, female life expectancy at birth in the most deprived areas fell by almost 100 days between 2012 to 2014 and 2015 to 2017
The change in LE between 2012 to 2014 and 2015 to 2017 was different across levels of deprivation. In general, males living in more deprived areas had either non-significant slight falls or gains in life expectancy, with gains becoming more substantial by decile 5 and then becoming statistically significant in areas located in deciles 9 and 10 (Figure 2). In decile 10, there was a statistically significant increase of 95 days in male life expectancy at birth, while males in decile 9 also achieved a significant gain of 91 days.
There was a statistically significant fall of almost 100 days in LE at birth among females living in the most deprived areas. This is in sharp contrast to the statistically significant gain of 84 days amongst females living in the least deprived areas. Taken together, this represents an increase of half a year in the absolute difference in LE between females living in the least and most deprived areas in England.
Figure 2: Change in life expectancy in days between 2012 to 2014 and 2015 to 2017: by sex and decile, England
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
- Females in decile 1 had a statistically significant decrease while females in decile 10 had a statistically significant increase in life expectancy.
- Males in deciles 9 and 10 had a statistically significant increase in life expectancy.
Download this chart Figure 2: Change in life expectancy in days between 2012 to 2014 and 2015 to 2017: by sex and decile, England
Image .csv .xlsFemales living in the most deprived areas can expect to live the shortest lives and live the smallest number of healthy years
Healthy life expectancy (HLE) at birth among males living in the most deprived areas in England was 51.7 years, compared with 70.4 years among the least deprived, almost two fewer decades of life in “Good” general health (Figure 3). Males in the least deprived 40% of areas were expected to live over their lifetimes more than 65 years, the traditional State Pension age, in “Good” health, while those in the most deprived 30% were expected to live fewer than 60 years in “Good” health.
The gap between adjacent deciles was largest between areas located within deciles 1 and 2; the latter were expected to live almost five years longer in “Good” health than males living in the most deprived areas. This demonstrates health outcomes were contrasting even between relatively deprived populations, as was also found for LE.
Figure 3: Male healthy life expectancy at birth and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents.
- The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 3: Male healthy life expectancy at birth and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Image .csv .xlsThe years spent in a poorer state of health for males were linked to level of deprivation exposure too: they fell progressively from 22.3 years among males living in the most deprived areas to 12.9 years among the least deprived areas (Figure 3).
Females in decile 1 could expect to live 52.0 years in “Good” health, compared with 70.4 years in decile 10, a noticeable difference, which is nearing two decades (Figure 4).
Figure 4: Female healthy life expectancy at birth and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
Life expectancy includes all usual residents.
The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 4: Female healthy life expectancy at birth and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Image .csv .xlsFemales in the least deprived 50% of areas were expected to live more than 65 years in “Good” health, while those in the most deprived 30% were expected to live fewer than 60 years in “Good” health (Figure 4).
The years spent in a poorer state of health for females were also linked to level of deprivation exposure: they fell from 26.7 years among females living in the most deprived areas to 15.8 years among the least deprived areas (Figure 4).
The gap between adjacent deciles was largest between decile 1 and decile 2 for females and similar to the equivalent gap for males. Decile 2 females were expected to live 4.9 years longer in “Good” health than females in decile 1.
The presence of the largest gap existing between decile 1 and 2 for both HLE as well as LE lends weight to the argument that the circumstances presented by falling below a given threshold of deprivation appear particularly harmful to health status.
The least deprived men and women at 65 years of age could expect to live 5.2 and 4.8 years longer respectively than their most deprived counterparts in 2015 to 2017
At 65 years of age, the men living in the most deprived areas were expected to live 15.8 years, 5.2 years fewer than the least deprived areas, who were expected to live 20.9 years (Figure 5).
Figure 5: Life expectancy at age 65 years by sex and selected national deciles of area deprivation, England, 2015 to 2017
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 5: Life expectancy at age 65 years by sex and selected national deciles of area deprivation, England, 2015 to 2017
Image .csv .xlsFor women, life expectancy (LE) at 65 years of age in the most deprived decile was 18.4 years, compared with 23.2 years among the least deprived, a gap of 4.8 years (Figure 5). The gaps between decile 9 and decile 10 (the deciles with the lowest levels of deprivation) and between decile 1 and decile 2 (the deciles with the highest levels of deprivation) were larger than differences between deciles located between 4 and 8.
It was useful to assess whether less deprived males outlived more deprived females at age 65 years also, as this has policy relevance in the areas of State Pension age reviews, fitness for work and care needs. It was found that men living in the 40% least deprived areas had statistically significant longer LE than women living in the 20% most deprived areas, a finding consistent with that at birth. The life expectancy of the intervening deciles can be found in the datasets accompanying this release.
There were statistically significant falls in life expectancy at age 65 years among women living in the 20% most deprived areas in England
The change in life expectancy between 2012 to 2014 and 2015 to 2017 was also linked to the level of deprivation exposed to at age 65 years, particularly noticeable towards the extremes of the deprivation scale.
Men living in the 30% most deprived areas suffered small non-significant falls in life expectancy ranging from less than a day to 14 days. However, men living in the 30% least deprived areas experienced statistically significant gains in life expectancy ranging from 50 days in decile 8 to 81 days in decile 10 (Figure 6). Men resident in decile 5 areas also achieved a statistically significant gain of 64 days, exceeding that of deciles 8 and 9.
Women at age 65 years living in the 20% most deprived areas suffered statistically significant falls in life expectancy ranging from 77 days in decile 2 to 84 days in decile 1. There were also non-significant falls in female life expectancy at age 65 years in deciles 3, 4, 5 and 6. Only women living in the least deprived areas located in decile 10 experienced a statistically significant increase in life expectancy of 60 days (Figure 6). Taken together, there has been a cumulative gain of two-fifths of a year for women in decile 10 over women in decile 1 between 2012 to 2014 and 2015 to 2017.
Figure 6: Change in life expectancy at age 65 years in days between 2012 to 2014 and 2015 to 2017: by sex and decile, England
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
- Females in decile 1 and 2 had a statistically significant decrease, while females in decile 10 had a statistically significant increase in life expectancy
- Males in decile 8, 9 and 10 had a statistically significant increase in life expectancy
Download this chart Figure 6: Change in life expectancy at age 65 years in days between 2012 to 2014 and 2015 to 2017: by sex and decile, England
Image .csv .xlsMen resident in the least deprived areas in England can expect 13.3 years of good health from 65 years of age, but only 5.8 years if resident in the most deprived areas
HLE at 65 years of age varied markedly by level of exposure to deprivation. Whereas men living in the least deprived areas could expect on average a healthy outlook for 13.3 years of their remaining life, this was only 5.8 years for those exposed to highest levels of deprivation (Figure 7).
Figure 7: Male healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents.
- The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 7: Male healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Image .csv .xlsThe pattern of HLE at 65 years of age across levels of deprivation for men was less regular than for life expectancy. However, the contrast across adjacent deciles was largest at 1.5 years between decile 1 and decile 2, and there was a consistent steep gradient between decile 1 and decile 5. There were also large gaps between deciles 4 and 5 and deciles 9 and 10. Men in decile 1 had a statistically significant lower HLE than all other deciles.
Women living in the least deprived areas were expected to live a further 13.8 years of their remaining life in good health, but this was only 6.9 years for women living in decile 1 (Figure 8).
Figure 8: Female healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents.
- The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Index of Multiple Deprivation 2015 (IMD15) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 8: Female healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, England, 2015 to 2017
Image .csv .xlsFor women, the pattern by deprivation exposure was more regular with HLE increasing incrementally as exposure to deprivation lessened. Women living in the most deprived decile had statistically significant lower HLE than all other deciles and significantly lower than men living in deciles 3 to 10.
There was less contrast in years lived in poorer states of health for women, but women living in the most deprived areas were living 2.1 years more in a poorer state of health than women living in the least deprived areas (Figure 8).
Back to table of contents5. Life expectancy and healthy life expectancy in Wales by the Welsh Index of Multiple Deprivation 2014 (WIMD14), 2015 to 2017
In Wales, the range in life expectancy at birth between the least and most deprived deciles was 8.8 years for males and 7.6 years for females in 2015 to 2017
The analyses of inequalities in Wales based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) should not be compared with England, and therefore stand alone. Please refer to the section ‘What are deprivation deciles?’ for further details on how the indexes of deprivation were constructed and the Health state life expectancies Quality and Methodology Information report.
Life expectancy (LE) at birth among males living in the most deprived areas in Wales was 73.6 years, compared with 82.4 years among the least deprived areas, a difference of 8.8 years in length of life (Figure 9).
Figure 9: Life Expectancy at birth by sex and selected national deciles of area deprivation, Wales, 2015 to 2017
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 9: Life Expectancy at birth by sex and selected national deciles of area deprivation, Wales, 2015 to 2017
Image .csv .xlsMales living in the least deprived 30% of areas were expected to live beyond the age of 80 years, while the remaining 70% were expected to fall short of this. The gap between adjacent deciles was largest between decile 1 and decile 2 (the two most deprived deciles), with the latter expected to live 1.4 years longer. Furthermore, there was also a sizeable gap in male LE at birth observed between decile 2 and decile 3 and between decile 9 and decile 10.
Males living in the most deprived decile had statistically significant lower life expectancy than all other deciles, while males living in the least deprived areas had statistically significant higher life expectancy than all other deciles. The life expectancy of the intervening deciles can be found in the datasets accompanying this release.
Females living in areas located in decile 1 were expected to live 78.2 years, while those living in areas located in decile 10 were expected to live 85.8 years, a difference of 7.6 years (Figure 9). Females resident in decile 1 areas had statistically significant shorter life expectancy than all other deciles, while females living in the least deprived areas had statistically significant longer life expectancy than all other deciles. The largest adjacent decile gaps were between deciles 1 and 2 and deciles 9 and 10 of almost 1.5 years, suggesting the extremes of the scale have stronger impacts on life expectancy than across the intervening deciles.
As in England, we conducted analyses to assess at what point on the deprivation scale do males outlive females to understand the importance of deprivation exposure in modifying the general comparison of LE between males and females. It was found that females resident in decile 1 areas were living statistically significant shorter lives than males living in the 50% least deprived areas (deciles 6 to 10). This shows that although in general females live longer than males, exposure to different levels of deprivation can alter this general pattern.
In Wales, falls in female life expectancy were observed since 2012 to 2014 among the 30% most deprived areas, but these were not statistically significant
The change in life expectancy between 2012 to 2014 and 2015 to 2017 was irregular across levels of deprivation in Wales and there were no statistically significant changes. The smaller populations in Wales mean LE estimates are less precise than in England, which hinder the detection of statistically significant changes, even though the changes themselves can be large and potentially meaningful.
Males living in the most deprived decile had a very small improvement in LE of only 3 days, whereas males living in the least deprived areas had an increase of 120 days. There was also a large fall of more than 200 days in decile 7, and approaching 150 days in decile 2, while decile 9 had the largest improvement of 126 days (Figure 10).
Figure 10: Change in life expectancy at birth in days between 2012 to 2014 and 2015 to 2017: by sex and decile, Wales
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 10: Change in life expectancy at birth in days between 2012 to 2014 and 2015 to 2017: by sex and decile, Wales
Image .csv .xlsThere was a contrary trajectory in LE for females living in the most deprived compared with the least deprived areas. The former suffered a fall of 136 days, while the latter gained 114 days, amounting to two-thirds of a year gained by those in decile 10 compared with those in decile 1. The largest fall was observed in decile 5, losing 224 days, while decile 6 females experienced the largest gain of 222 days; an interesting contrast among those residing in the middle of the deprivation scale. However, all these changes were not statistically significant.
Females in the most deprived areas are living close to 11 years on average more in a poorer state of health than females in the least deprived areas in Wales
Healthy life expectancy (HLE) at birth for males was lowest at 50.6 years in the most deprived areas and highest at 68.8 years in the least deprived areas, a difference of 18.2 years (Figure 11). The largest adjacent gap for males at birth was 3.6 years between decile 1 and decile 2, but a large 3.0 years gap also existed between decile 9 and decile 10.
Only men living in the 30% least deprived areas (those living in areas located in deciles 8, 9 and 10) were expected to live more than 65 years in “Good” health, while the most deprived 40% of areas (those living in areas located in deciles 1, 2, 3 and 4) were expected to live fewer than 60 years in “Good” health.
Figure 11: Male healthy life expectancy at birth and years lived in poorer states of health: 2015 to 2017: by national deprivation deciles, Wales, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents. 2. The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 11: Male healthy life expectancy at birth and years lived in poorer states of health: 2015 to 2017: by national deprivation deciles, Wales, 2015 to 2017
Image .csv .xlsHLE at birth for females was 50.3 years in decile 1. This was 18.4 years fewer than decile 10, which was 68.7 years (Figure 12). The largest gap between adjacent deciles was between deciles 1 and 2 at 4.8 years of healthy life, suggesting that even among relatively deprived populations, the extent of deprivation exposure is meaningful for health status in Wales as well as in England.
Figure 12: Female healthy life expectancy at birth and years lived in poorer states of health: 2015 to 2017: by national deprivation deciles, Wales, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents.
- The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 12: Female healthy life expectancy at birth and years lived in poorer states of health: 2015 to 2017: by national deprivation deciles, Wales, 2015 to 2017
Image .csv .xlsAlthough LE among females in the most deprived areas was 7.6 years shorter than females in the least deprived areas, females in the most deprived areas are likely to spend close to 11 years more in a poorer state of health than those living in the least deprived areas (Figure 12). As HLE is only 50.3 years among females living in the most deprived areas, it is likely such females experience the onset of certain types of health conditions harmful to health-related well-being much earlier than in other populations in Wales.
The inequality in life expectancy at age 65 years between the least and most deprived deciles is larger for women than men in Wales
At 65 years of age, men living in the most deprived areas were expected to live 15.7 years, 4.6 years fewer than in the least deprived areas, who were expected to live 20.3 years (Figure 13).
For women, LE at 65 years of age in the most deprived decile was 17.7 years, compared with 22.9 years among the least deprived, a gap of 5.2 years (Figure 13).
Figure 13: Life expectancy at age 65 years by sex and selected national deciles of area deprivation, Wales, 2015 to 2017
Source: Office for National Statistics
Notes:
- Life expectancy (LE) includes all usual residents.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 13: Life expectancy at age 65 years by sex and selected national deciles of area deprivation, Wales, 2015 to 2017
Image .csv .xlsMales living in the 50% least deprived areas had statistically significant longer LE than females living in the 10% most deprived areas at age 65 years.
For women, there were large gaps in LE at age 65 between deciles 1 and 2 and deciles 9 and 10, which exceeded a year and were much larger than between any other deciles, showing disproportionate difference in outcomes at the extremes of the scale.
Men at age 65 years living in the 20% least deprived areas gain more than 100 days of life since 2012 to 2014, while women living in the most deprived areas lose 94 days
The change in life expectancy between 2012 to 2014 and 2015 to 2017 was irregular in Wales across levels of deprivation as at birth and there were no statistically significant changes for both men and women. Men living in the most deprived decile gained 58 days, but those in decile 2 lost almost a third of a year. Men in deciles 9 and 10 gained 113 and 117 days respectively (Figure 14). There was also a sharp contraction in decile 7 and a large gain in decile 4.
Figure 14: Change in life expectancy at age 65 years in days between 2012-2014 and 2015-2017: by sex and decile, Wales
Source: Office for National Statistics
Notes:
Life expectancy (LE) includes all usual residents.
Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 14: Change in life expectancy at age 65 years in days between 2012-2014 and 2015-2017: by sex and decile, Wales
Image .csv .xlsFor women, the largest change occurred in the most deprived decile, with women losing 94 days. In general, the change in women’s LE was smaller than for men.
A lessening in deprivation was not always associated with a corresponding rise in healthy life expectancy at age 65 years in Wales
At 65 years of age, men in the most deprived areas were expected to live only 5.7 years in good health, only half as long as those living in the least deprived areas (11.3 years). The relationship between HLE and area deprivation though was somewhat more irregular in Wales, as the highest HLE at 65 years of age was observed in decile 8 at 11.9 years (Figure 15). This was caused by the modelled self-reported health measures being highest in decile 8 for ages 75 years and over.
Figure 15: Male healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, Wales 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- Life expectancy (LE) includes all usual residents.
- The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
- Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 15: Male healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, Wales 2015 to 2017
Image .csv .xlsFor women at age 65 years, the pattern of HLE across levels of area deprivation was also less regular than at birth (Figure 16).
Figure 16: Female healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, Wales 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
Life expectancy (LE) includes all usual residents.
The health state prevalence estimates used to estimate healthy life expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents’ address.
Deprivation deciles are based on the Welsh Index of Multiple Deprivation 2014 (WIMD14) which is the official measure of relative deprivation. Decile 1 represents the most deprived and decile 10 represents the least deprived.
Download this chart Figure 16: Female healthy life expectancy at age 65 years and years lived in poorer states of health: by national deprivation deciles, Wales 2015 to 2017
Image .csv .xlsHLE among women in the most deprived areas was 5.9 years, with a gap of 6.7 years compared with women living in the least deprived areas whose HLE was 12.6 years. There was a marked jump in HLE between decile 1 and decile 2 of 2.7 years, showing a sharp contrast between relatively deprived women.
Although life expectancy at 65 years of age among women in the most deprived decile was 5.2 years shorter than in the least deprived areas, they spend 1.5 years longer in a poorer state of health than those living in the least deprived areas (Figure 16). For women, the years lived in poorer states of health from 65 years of age ranged from 11.8 years in decile 1 to 9.3 years in decile 9. For men, it ranged from 10.0 years in decile 1 to 7.4 years in decile 8. In general, men spend fewer years in poorer states of health than women, partly a reflection of their shorter life expectancy.
Back to table of contents6. The Slope Index of Inequality for life expectancy and healthy life expectancy in England
The gap in the years lived in good health from birth as measured by the Slope Index of Inequality was more than twice as wide as that for life expectancy.
In 2015 to 2017, the inequality in life expectancy (LE) in England for males at birth, as measured using the Slope Index of Inequality (SII), stood at 9.4 years whereas for females the SII was 7.4 years.
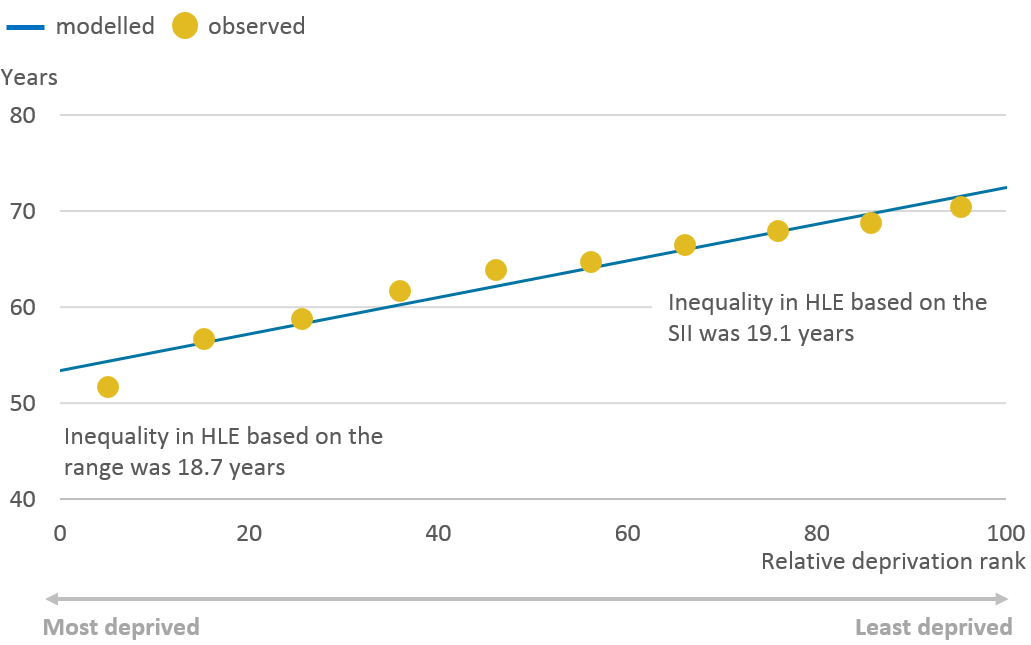
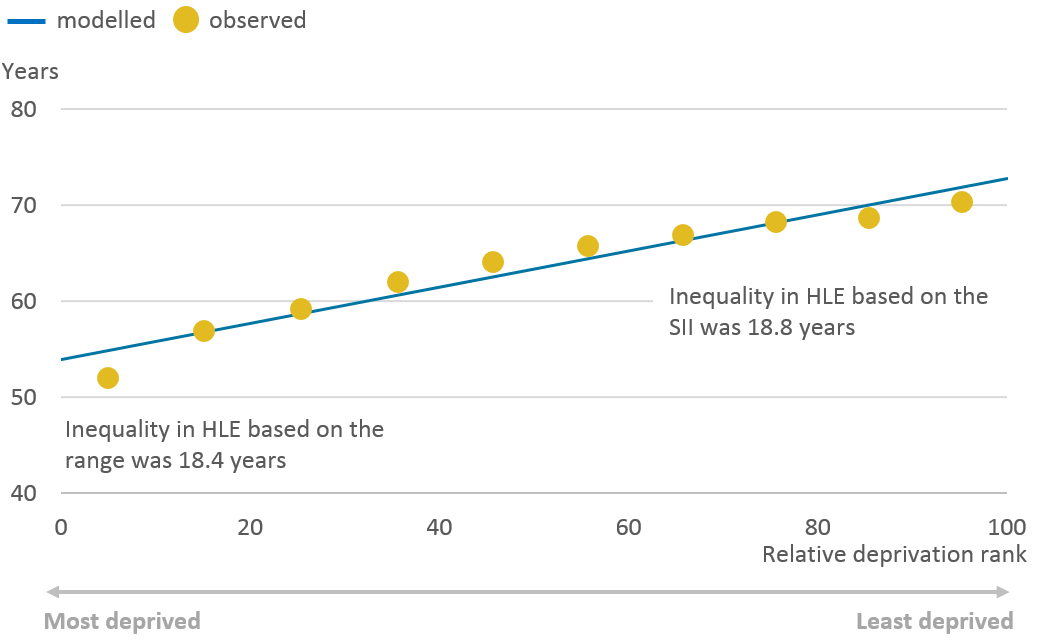
While there was a statistically significant higher inequality in male LE compared with female LE at birth and at age 65 years, it was not found to be significant for healthy life expectancy (HLE). The SII at birth was 19.1 years for males and 18.8 years for females (Figures 17 and 18).
Figure 17: Slope index of inequality in male healthy life expectancy at birth: England, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
The health state prevalence estimates used to estimate Healthy Life Expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents' address.
Slope Index of Inequality (SII) is calculated by taking the difference between the extremes of a population weighted regression line of best fit.
Download this image Figure 17: Slope index of inequality in male healthy life expectancy at birth: England, 2015 to 2017
.png (37.7 kB) .xls (39.9 kB)
Figure 18: Slope index of inequality in female healthy life expectancy at birth: England, 2015-2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
The health state prevalence estimates used to estimate Healthy Life Expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents' address.
Slope Index of Inequality (SII) is calculated by taking the difference between the extremes of a population weighted regression line of best fit.
Download this image Figure 18: Slope index of inequality in female healthy life expectancy at birth: England, 2015-2017
.png (39.5 kB) .xls (28.7 kB)As can be observed from Figures 17 and 18, the linear model used is a good fit for the data, suggesting a meaningful relationship between HLE and area deprivation. The SII in HLE at birth was 0.4 years wider than the range for both sexes, showing the value of estimating the inequality that takes account of the inequality between all deciles, weighted by their population size. The socioeconomic inequality in the years lived in good health was more than twice as wide as life expectancy, showing that there is greater disparity in the quality of years lived.
At 65 years of age, the SII in LE for men was 4.9 years compared with 4.5 years for women, suggesting sizeable socioeconomic inequalities persist at 65 years of age as found in alternative measures of socioeconomic position. The inequality in HLE at 65 years of age for men was 7.0 years and for women 7.1 years, showing the quality of the years spent during retirement is also patterned in favour of less deprived populations.
Back to table of contents7. The Slope Index of Inequality for life expectancy and healthy life expectancy in Wales
The inequality in male and female healthy life expectancy at birth in Wales spans more than 18 years for males and 19 years for females
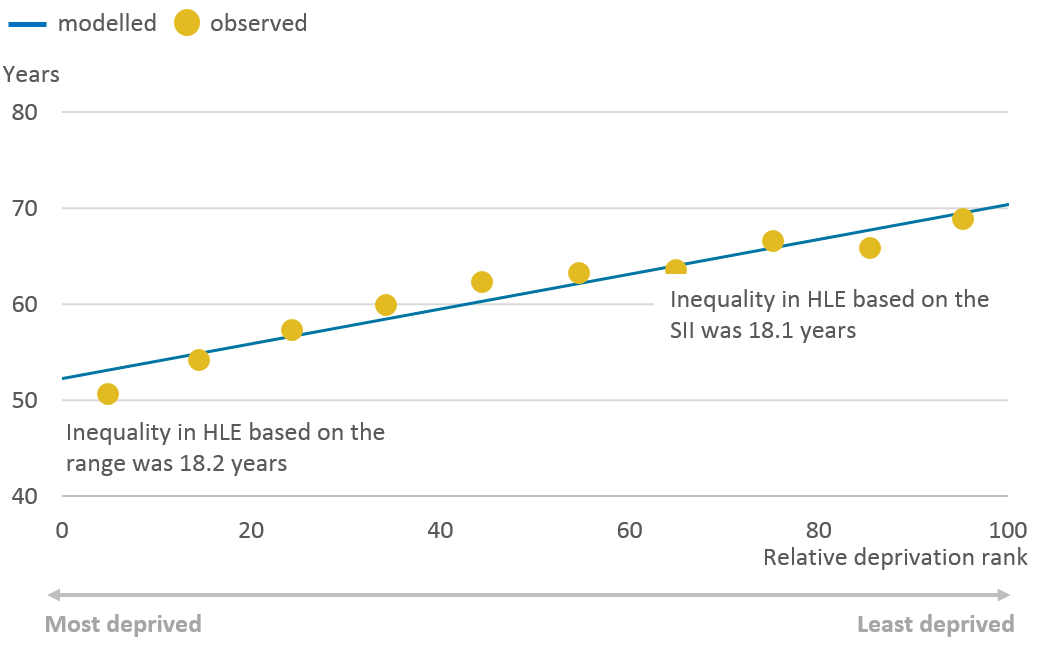
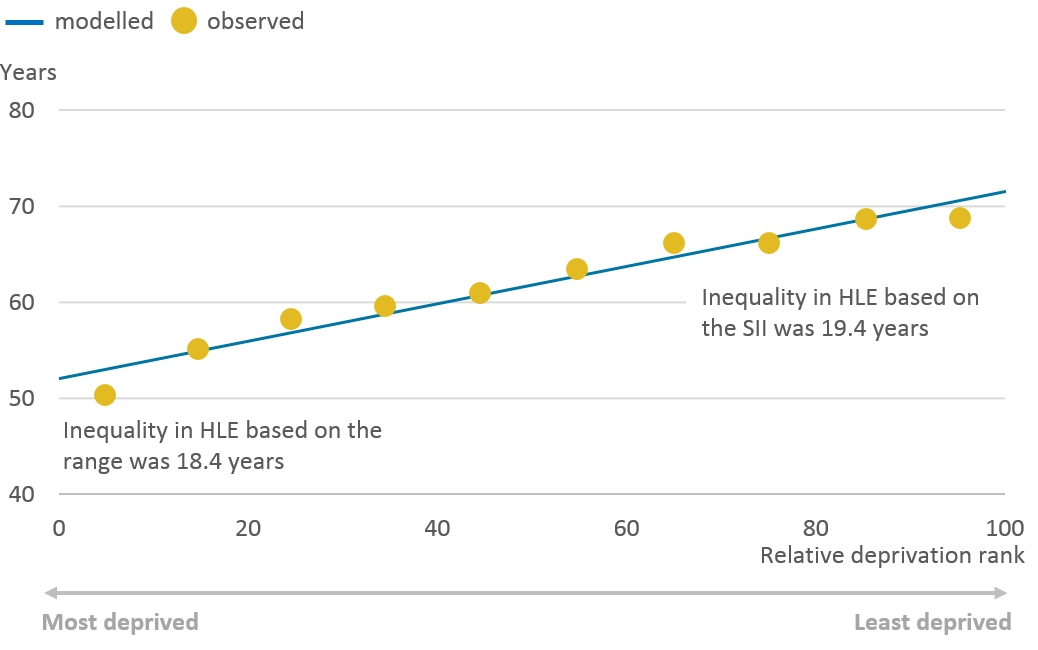
In 2015 to 2017, the inequality in male life expectancy (LE) at birth in Wales stood at 9.0 years, a statistically significant higher inequality to that of females, which stood at 7.5 years. Healthy life expectancy (HLE) at birth had a more substantial gap, but the inequality was reversed with females having the larger inequality, at 19.4 years compared with 18.1 years for males (Figures 19 and 20).
Figure 19: Slope index of inequality in male healthy life expectancy at birth: Wales, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
- The health state prevalence estimates used to estimate Healthy Life Expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents' address.
- Slope Index of Inequality (SII) is calculated by taking the difference between the extremes of a population weighted regression line of best fit.
Download this image Figure 19: Slope index of inequality in male healthy life expectancy at birth: Wales, 2015 to 2017
.png (39.2 kB) .xls (28.7 kB)
Figure 20: Slope Index of Inequality in female healthy life expectancy at birth: Wales, 2015 to 2017
Source: Office for National Statistics - Annual Population Survey, 2011 Census
Notes:
The health state prevalence estimates used to estimate Healthy Life Expectancy (HLE) are sourced from Annual Population Survey (APS) data. The APS excludes residents of communal establishments except NHS housing and students in halls of residence where inclusion takes place at their parents' address.
Slope Index of Inequality (SII) is calculated by taking the difference between the extremes of a population weighted regression line of best fit.
Download this image Figure 20: Slope Index of Inequality in female healthy life expectancy at birth: Wales, 2015 to 2017
.png (38.7 kB) .xls (28.7 kB)While the inequality as measured by the range and SII were similar for males, the range was found to underestimate the inequality in HLE for females by a year.
At 65 years of age, inequalities in life expectancy in Wales persisted with a gap of 4.6 years for both men and women, showing an alignment in the magnitude of inequality at older ages in Wales. At 65 years of age, the gap in HLE was also wider for women at 6.2 years compared with 5.1 years for men.
Back to table of contents8. Comparing inequalities in life expectancy and healthy life expectancy between 2012 to 2014 and 2015 to 2017, England
The socioeconomic inequality in female life expectancy at birth significantly widened by 0.5 of a year in England
While the range and Slope Index of Inequality (SII) for life expectancy (LE) and healthy life expectancy (HLE) are important for a given point estimate such as that in 2015 to 2017, the change from the most recent non-overlapping period (2012 to 2014) is also important to consider, as it provides an opportunity to assess progress in narrowing the gap (PDF, 129KB). Table 1 contains the SII in England for LE and HLE for the periods 2012 to 2014 and 2015 to 2017.
| 2012 to 2014 | 2015 to 2017 | ||||||
|---|---|---|---|---|---|---|---|
| SII (years) | Range (years) | SII (years) | Range (years) | SII difference | Range difference | ||
| Males at birth | |||||||
| LE | 9.1 | 9.1 | 9.4 * | 9.3 | 0.3 | 0.2 | |
| HLE | 18.8 | 18.5 | 19.1 | 18.7 | 0.2 | 0.2 | |
| Men at age 65 | |||||||
| LE | 4.7 | 4.9 | 4.9 * | 5.2 | 0.2 | 0.3 | |
| HLE | 6.7 | 6.6 | 7.0 | 7.5 | 0.4 | 0.9 | |
| Females at birth | |||||||
| LE | 6.9 | 7.0 | 7.4 * | 7.5 | 0.5 | 0.5 | |
| HLE | 19.7 | 19.2 | 18.8 | 18.4 | -0.9 | -0.8 | |
| Women at age 65 | |||||||
| LE | 4.2 | 4.4 | 4.5 * | 4.8 | 0.3 | 0.4 | |
| HLE | 7.3 | 7.5 | 7.1 | 6.9 | -0.3 | -0.6 | |
Download this table Table 1: Comparison of the Slope Index of Inequality and range in life expectancy and healthy life expectancy at birth and at age 65 by sex
.xls .csvThere was a statistically significant increase in the inequality in male LE at birth of 0.3 years, with the SII growing from 9.1 years in 2012 to 2014 to 9.4 years in 2015 to 2017 (Table 1). There was also a statistically significant increase in the socioeconomic inequality in LE for men at 65 years of age of 0.2 years, rising to 4.9 years in 2015 to 2017 from 4.7 years in 2012 to 2014. The increase in the inequality was the result of statistically significant gains in the 20% least deprived areas in the presence of a very small non-significant improvement in the most deprived decile and a non-significant decrease in decile 2.
Female LE at birth was also observed to have a statistically significant increase in the inequality of 0.5 years, exceeding the increase experienced by males and thereby contracting the difference in the scale of the inequality between males and females. In the period 2012 to 2014, the SII was 6.9 years but this grew to 7.4 years in 2015 to 2017. For women, there was a statistically significant rise in the socioeconomic inequality in LE at 65 years of age as measured by the SII, increasing to 4.5 years in 2015 to 2017, from 4.2 years in 2012 to 2014.
In general, the change in LE at birth for females across all deciles other than decile 4 was less favourable than for males, in that it did not improve as much when it increased, and decreased by more when it worsened, and in some cases male life expectancy rose when female life expectancy fell. At age 65 years, men’s trajectory in life expectancy was also more favourable than women across all deciles. The effect was to close the gap between male and female LE at birth and at age 65 years across deprivation deciles.
There has been a pattern of increasing growth in the inequality in female life expectancy at birth since 2011 to 2013, the first data point in the current series. This is caused by consecutive statistically significant falls in female life expectancy at birth among females living in the most deprived areas together with statistically significant rises among females living in the least deprived areas. The growth in the inequality observed, suggests the falling improvement in mortality reductions is more intensively concentrated in deprived areas of England, as was found in the recent Public Health England Review of recent trends in mortality in England (PDF 2.93MB).
The change in the inequality in male and female HLE at birth since 2012 to 2014 was divergent but not statistically significant (Table 1). For males, the inequality as measured by the SII grew from 18.8 years in 2012 to 2014, to 19.1 years in 2015 to 2017. However, for females the SII decreased by 0.9 years over the same time period. The fall in the inequality in female HLE at birth was caused by a fall in deciles 9 and 10.
At age 65 years the inequality in HLE grew for men and reduced for women, but these changes were not statistically significant.
Back to table of contents9. Comparing inequalities in life expectancy and healthy life expectancy between 2012 to 2014 and 2015 to 2017, Wales
There was a non-significant increase in the inequality in life expectancy at birth by more than half a year for females in Wales
The inequality in male life expectancy (LE) at birth increased in Wales by half a year; the Slope Index of Inequality (SII) widened from 8.5 years in 2012 to 2014, to 9.0 years in 2015 to 2017 (Table 2). However, this half of a year increase was not statistically significant. The SII in female LE at birth also increased from 6.9 years to 7.5 years over the same time period, but again this 0.6 of a year increase was not statistically significant.
| 2012 to 2014 | 2015 to 2017 | ||||||
|---|---|---|---|---|---|---|---|
| SII (years) | Range (years) | SII (years) | Range (years) | SII difference | Range difference | ||
| Males at birth | |||||||
| LE | 8.5 | 8.5 | 9.0 | 8.8 | 0.5 | 0.3 | |
| HLE | 18.0 | 17.3 | 18.1 | 18.2 | 0.2 | 0.9 | |
| Men at age 65 | |||||||
| LE | 4.4 | 4.4 | 4.6 | 4.6 | 0.3 | 0.2 | |
| HLE | 5.7 | 4.8 | 5.1 | 5.6 | -0.6 | 0.8 | |
| Females at birth | |||||||
| LE | 6.9 | 6.9 | 7.5 | 7.6 | 0.6 | 0.7 | |
| HLE | 20.5 | 19.3 | 19.4 | 18.4 | -1.1 | -0.9 | |
| Women at age 65 | |||||||
| LE | 4.6 | 4.9 | 4.6 | 5.2 | 0.1 | 0.3 | |
| HLE | 7.2 | 6.5 | 6.2 | 6.7 | -1.0 | 0.2 | |
Download this table Table 2: Comparison of the Slope Index of Inequality and range in life expectancy and healthy life expectancy at birth and at age 65 by sex
.xls .csvAt 65 years of age the pattern of change across deciles for men was more favourable than at birth and particularly more favourable than for women. The SII, however, increased from 4.4 years in 2012 to 2014, to 4.6 years in 2015 to 2017; this increase was not statistically significant. For women at age 65 years, the SII in LE rose very slightly (Table 2).
There was a non-significant narrowing in the inequality in healthy life expectancy at birth by more than a year for females in Wales
For females at both birth and aged 65 years the inequality in healthy life expectancy contracted by more than a year, although this was not statistically significant (Table 2). At birth, the SII for healthy life expectancy (HLE) narrowed from 20.5 years in 2012 to 2014, to 19.4 years in 2015 to 2017, while at 65 years of age it narrowed from 7.2 years to 6.2 years.
For males at birth, the SII saw a 0.1 of a year increase from 2012 to 2014 reaching 18.1 years in 2015 to 2017; at 65 years of age it narrowed by 0.6 of a year standing at 5.1 years in 2015 to 2017. The changes observed in the inequality for males were also not statistically significant.
Back to table of contents10. Quality and methodology
The Health state life expectancies Quality and Methodology Information report contains important information on:
- the strengths and limitations of the data and how it compares with related data
- users and uses of the data
- how the output was created
- the quality of the output including the accuracy of the data
Calculating health state life expectancy
The data used in calculating the prevalence of health states was obtained from the Annual Population Survey (APS) and the 2011 Census. The APS data were aggregated over a three-year period to achieve sufficiently large sample sizes to enable meaningful statistical comparison at subnational level. 2011 Census data was used for imputation and in modelling health states. Further details can be found in the Health state expectancies Quality and Methodology Information report.
The prevalence of “Good” general health and disability-free among males and females resident in private households in England was compared across areas. HLE was then calculated using the Sullivan method (PDF, 1.2MB), which combines prevalence data with mortality and mid-year population estimates (MYE) over the same period and geographical coverage to calculate estimates of life expectancy (LE), healthy life expectancy (HLE) and disability-free life expectancy (DFLE) by age and sex (for more information, see the ONS life table template).
The APS provides prevalence information for those aged 16 years and over. We are able to estimate lower age groups by using a census imputation method.
Results are presented with 95% confidence intervals in datasets to help interpretation. Confidence intervals in this statistical bulletin indicate the uncertainty surrounding the health state life expectancy measures (healthy life expectancy and disability-free life expectancy) and allow more meaningful comparisons between areas. When comparing two estimates, non-overlapping confidence intervals are indicative of statistical significance.
Indices of Multiple Deprivation
The Indices of Multiple Deprivation (IMD) are a score based on the area as a whole and not everyone within a Lower layer Super Output Area (LSOA) necessarily experiences the same level or type of deprivation. For example, some unemployed individuals live in less deprived LSOAs, while some higher-income individuals live in more deprived LSOAs. Similarly, deciles are a broad grouping and the levels of deprivation and the underlying factors determining the LSOA-level deprivation score will vary within the decile. Those LSOAs at the higher and lower end of each specific decile may vary considerably from each other. The widest variation is generally found between deciles 1 and 10.
England’s measure of deprivation is based on the Index of Multiple Deprivation (IMD) 2015; this index is calculated using seven domains:
- income
- employment
- education, skills and training
- health and disability
- crime
- barriers to housing and services
- living environment
Wales’s measure of deprivation is based on the Welsh Index of Multiple Deprivation (WIMD) 2014 eight domains:
- income
- employment
- health
- education
- access to services
- community safety
- physical environment
- housing
Slope Index of Inequality
The Slope Index of Inequality (SII) was used to assess the absolute inequality in life expectancy (LE) and each health state life expectancy between the least and most deprived deciles. This indicator measures the gaps by taking account of the inequality across all adjacent deciles of relative deprivation, rather than focusing only on the differencing of the two extremes.
To calculate the Slope Index of Inequality
Deciles were ordered by decreasing area deprivation, that is, from the most to the least deprived. The fraction of the total population in each decile (f) was calculated. The cumulative frequency (ci), that is, the cumulative sum of the population in successively less deprived deciles, was also obtained and the relative deprivation rank (x) for each decile was calculated as:
This formula calculates the relative deprivation rank for use in the Slope Index of Inequality calculation.
The SII (a line of best fit) was then estimated by regressing the outcome measures (LE, HLE and DFLE) separately against the relative deprivation rank (x), weighted by the population in each decile.
Confidence interval details for SII indicators
The confidence intervals for the SII are calculated using a simulation program. Simulation is a method used to estimate the degree of uncertainty for measures where the statistical distributions underpinning the measure are too complex to analyse mathematically.
For each decile, the life expectancy (LE), healthy life expectancy (HLE) and disability-free life expectancy (DFLE) has been calculated along with its standard error (SE). These SEs give information about the degree of uncertainty around each of the health state life expectancy values: essentially it describes a statistical distribution for each decile.
Using a random number generating algorithm, a random value is taken from each decile LE and HLE distribution and the SII recalculated. This is repeated many times (for example, 10,000), to build up a distribution of SII values based on random sampling from the decile LE distributions. The 2.5% and 97.5% values from this distribution of SII values is then reported as the 95% confidence interval for the SII, rather than that based on 10 observations representing the deciles.
Note that previously the confidence intervals were calculated based purely on the SII regression slope, ignoring the distributional information about the decile LEs and HLEs. This method generally overestimated the width of the confidence intervals, that is, it was overly conservative in most cases. The current method allows greater discrimination between areas and over time and greater opportunity to detect significance change over time.
Back to table of contents
